If all we need is to see the body to know it, what do we know? Throughout time, western medicine has sought to see deeper and deeper into the human body. Science has sought to develop technologies that help make the body visible, from X-rays to MRIs and CAT scans to microscopic imaging of bacteria and blood cells. The motivation? To sharpen its vision and, thereby its clarity of the human body’s internal workings. The better medicine can see the body, the better it can know the innate truth of the body– the better it can then diagnose, treat, and heal the body. These technologies seek to create images of the body, mainly its internal workings, so that they can be seen objectively and interpreted. I want to challenge the idea that the medical image is an objective image. Is the image of a broken arm just that, an image of a broken radius or ulnar bone? Or is it something more?
Michel Foucault identified this objective way of seeing the body as the “medical gaze” in The Birth of the Clinic. Foucault explains that the practitioner is trained to “subtract[s] the individual, with his particular qualities,” in order to isolate “the course of the disease [so it] is not interrupted or disturbed by the patient” (14). In other words, the western medical practitioner is trained to focus on the disease or injury so they can clearly assess the problem and not become distracted by the patient. As technologies developed, this gaze deepened. X-ray and MRIs allowed organs and bones to be visible and separated from the patient. The practitioner views these through this medical gaze in which they have been trained. The patient is subtracted, and the broken radius illuminated. In this essay, I pose the question, can the patient be subtracted? I want to suggest that in an X-ray image that shows a broken radius for example, the patient remains.
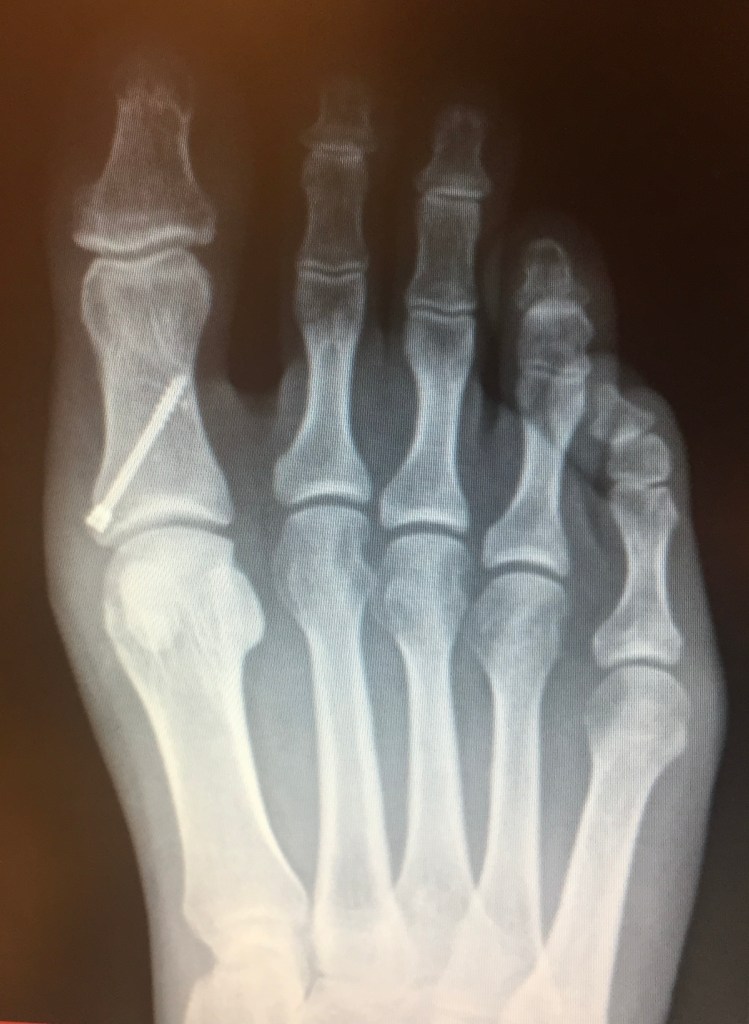
Take the cover image of this piece as an example. When the practitioner sees it through his medical gaze, he sees a successfully placed surgical screw into the proximal phalanx of the great toe on a right foot. Through this gaze, he doesn’t see the pain of the patient. He doesn’t see the ways it impacts her daily life, the pain in each step taken with that foot. He doesn’t see how it complicates the choices of where to park at a store, and limits her choice of footwear to one set of oversized tennis shoes. The meanings of medical images matters because if he saw what she sees, perhaps he would make time for practical questions of mobility or questions about healing from having such a surgery. He might shift his gaze from the objective success of the surgery to the subjective lived experience and impact it has on his patient. It might change the way he approaches the clinical conversation.
The trouble with considering the body from a place of objectivity is that we are always there. The person is embedded in this image of the foot. The subjective experiences, the lived realities of our internal bodily experiences are always attached to those medical images, no matter how hard the medical gaze attempts to subtract it. Would it not make sense that embracing this could lead to a better patient experience? Could seeing this complexity of the body, improve healing the body? What might we come to know about healing the human body if only we broadened the medical gaze?
This medical gaze is, of course, something that exists within the specific place of the clinic. When we change the place where these images are viewed, from a medical place, such as the doctor’s office or the lab, to the patient’s home, the meanings and interpretations of these images change. Likewise, as Annemarie Mol suggests with her book the body multiple, “in practice the body and its diseases are more than one, but this does not mean that they are fragmented into being many” (viii). It is important to realize that as the medical gaze considers the injury or illness of a person, that foot, for example, still belongs to a person even when isolated in a medical image and viewed through the medical gaze.
In the home, in the clinic, in the lab – injury and disease are seen differently. In the clinic it is viewed objectively as a set of symptoms. In the home it is an inability to wear certain shoes or do a certain activity. In the lab it is a microorganism made visible through a microscope. It is this multiplicity of disease that begs the question, how might these lines blur for the patient? Furthermore, when does the practitioner need to consider this?
Considering that there are more meanings to these images than what is apparent when viewing them as objective representation of a human body part suggests that even in these objective places, these meanings persist.
The medical image and the viewing of that image is perhaps one of these moments. The viewing of medical images through the medical gaze can create distance between the patient and the practitioner because it removes the patient from the practitioner’s focus, replacing it with an objective image. Considering the depth of meaning embedded in these images, as discussed above, might refocus the practitioner onto the patient.
This argument also illuminates how complicating the medical image might impact the patient experience. If in one place, such as the home, the patient sees this subjective hidden narrative of illness experience, in what ways does it remain even in places in which it is not considered or not seen? Such as the clinic? What would this mean in terms of the communication between the practitioner and the patient?
Through this framework of thinking differently about the medical image different ways of approaching the patient and the clinical appointment might be possible. It strengthens the connection between the image and the patient, allowing for the practitioner to remember that these images are part of a person. They are not an objective image but contain the interrupted life of an individual seeking help. Therefore, perhaps when discussing and reviewing them through this mindset, a more holistic patient centered approach is more readily enacted in clinical conversation.
I leave you with these final questions:
As a patient, how might this way of thinking help to make sense of the feelings and experiences you have in the clinic?
As a practitioner, in what ways might this way of thinking impact your clinical approach to the patient, if at all?
Works Cited:
Foucault, Michel. The Birth of the Clinic: An Archaeology of Medical Perception. 1963. Vintage, 1994.
Mol, Annemarie. The Body Multiple: Ontology in Medical Practice. Duke University Press, 2002.
Image Credit: