It’s the second week of my rotation with a reproductive health advocacy organization. On my desktop, a grid of squares, icons of faces interspersed with actual faces, populate the screen. They are from the east and west coast, and some United States territories. More than half of them are Black or Latinx. Each of them has watcheda curriculum developed by the organization that is intended to bring awareness to newborn screening, focusing on its histories, practices, and processes. One of my first assignments is to watch this recording of this post-curriculum focus group with the doulas, where the organization invited them to share their thoughts and experiences.
The first questions posed to the group are straightforward: how did they feel about the curriculum? What did they learn from it? The first responses are warm; one doula shares that she learned a lot, and the curriculum inspired her to learn more about the newborn screening process in her state. Another echoes this statement, acknowledging how surprised she was at the fact that this is something every newborn has engaged with in the United States.
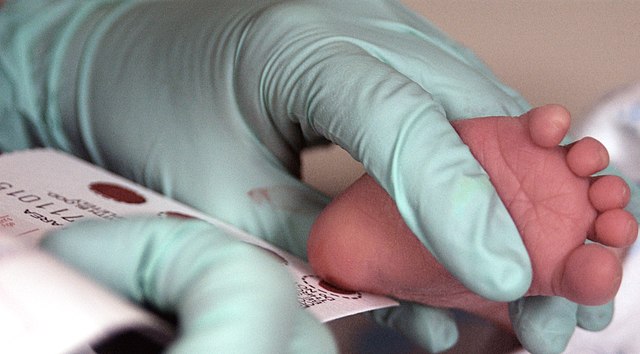
It is not just doulas who encounter the newborn screening program with surprise. Despite the fact that nearly every child in the United States has engaged with the newborn screening program, few people who have given birth can recall this test as part of their child’s routine follow-up care. It is not necessarily surprising that a screening test so ubiquitous could fly under the radar for so many, either: using relatively simple medical tools, newborn screening is a set of tests done to detect infants who may have been born with a defined list of heritable or congenital conditions. Materially, newborn screening consists of a few different tests: a brief prick of the newborn’s heel, followed by the collection of blood on a piece of paper; pulse oximetry to detect congenital heart defects; and the use of a specialized device to test for hearing. These techniques easily blend in with the infrastructure around contemporary birth practice. For the many babies whose screening results are negative, the norm is little to no necessary follow-up. As a result, these techniques easily blend in with the infrastructure around contemporary birth practice.
The value in newborn screening best materializes when a screening result is positive. Newborn screening is understood as a preventative program: by screening all newborns, we can identify those in which early intervention may lessen the impact of the condition over time. Newborn screening’s preventative nature is operationalized by stakeholders and other advocates to justify it. The doulas in this group understood, and reiterated this principle.
However, some of the doulas sought to complicate this claim. Shortly after the initial comments, one doula within the grid spoke up. “There is concern on whether this test is really for us,” she shared, “those of us who are melanated, or not of Caucasian ancestry”. This comment unraveled a broader thread, where many of the doulas themselves shared their own questions about both what conditions are tested for, as well as the structural barriers present to having their clients’ needs heard.
There are many layers to this part of the conversation. It is a myth that conditions like Cystic Fibrosis and PKU, the condition which instigated newborn screening in the United States, are exclusively seen in white individuals. That being said, there are disparities evident in the newborn screening process for identification and subsequent follow-up for these conditions in black newborns which can have profound consequences for disease trajectory (McColley et al., 2022). Such disparities in the screening alone don’t account for the broader experience of institutional racism and its material impacts on black birthing parents and their children.
These doulas’ remarks recall Timmermans and Buchbinder’s (2013) discussions of “potentializing” newborn screening. Using a frame of semiotics, they describe newborn screening as a political project built on potentialities: of early detection, of harm reduction, of positive outcome. Integral to Timmermans and Buchbinder’s argument is the fact that this potentializing message is often separated from the lived processes of newborn screening, where state laboratories are under-funded and under-staffed, and false positives are an inherent part and possibility of the screening process that create their own unique form of distress for parents. As the doulas in this focus group make evident, early detection does not erase the ills and errors of an inequitable medical system.
What does it look like to de-potentialize newborn screening? What happens if we are more honest about its challenges, its pitfalls, its limitations? As I’ve gone through my genetic counseling training, how I operationalize my knowledge about newborn screening as a doula has evolved. I am more nuanced in my delivery, aware of the signals and beliefs laden the presentation of newborn screening as an uncritical “good”. I acknowledge the rarity that a screen may come back positive, but discuss the systems available to confirm and follow up on a positive, flaws and all. With my awareness of its pitfalls, I feel a sense of responsibility for my doula clients; it aches from the same place that has seen careless providers disregard a patients’ discomfort, before I intervene; the same part of me that has felt a flash of rage when providers and nurses watch a patients’ fetal monitor instead of watching the patient, themselves. In this sense–and I believe this is what the doulas were getting at–newborn screening is one of many portals into the way our work reaches the edges of protecting patients against monstrously large pitfalls in supporting pregnant people and their families. To be transparent about that–with ourselves, with our patients–is harsh, and painful. Potentializing newborn screening, then, isn’t just about presenting the process as undeniably positive: it is also about trying to own the pieces of the perinatal care continuum which are successful, when so much of what stands demands revision.
Even still, I remain stuck in an odd kind of professional liminality: somewhere between my own investment in the potentializing of newborn screening, and a personal, intimate awareness of how contemporary perinatal health care fails pregnant people and their families.
Sources
McColley, Susanna A., Stacey L. Martiniano, Clement L. Ren, Marci K. Sontag, Karen Rychlik, Lauren Balmert, Alexander Elbert, Runyu Wu, and Philip M. Farrell. “Disparities in first evaluation of infants with cystic fibrosis since implementation of newborn screening.” Journal of Cystic Fibrosis (2022).
Timmermans, Stefan, and Mara Buchbinder. “Potentializing newborn screening.” Current Anthropology 54, no. S7 (2013): S26-S35.
Photo Credit
U.S. Air Force photo/Staff Sgt Eric T. Sheler. “Phenylketonuria Testing.” Wikimedia Commons, 12 December 2007.